Here are a few descriptions of many of the procedures we do:


- Home
- Who We Are
- Who We Are
- Dr. Sasha Stasko
- Team
- What We Do
- What We Do
- Periodontal Disease
- Periodontal Disease
- Comprehensive Care
- Periodontal Flap Surgery
- Dental Implants
- Dental Implants
- Dental Implants
- Immediate Temporization of Implants
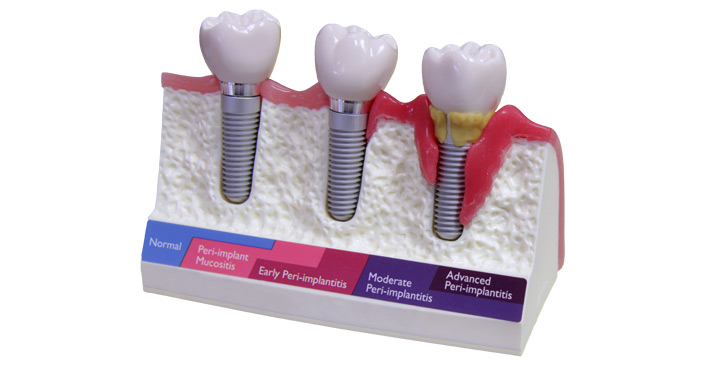
- Peri-Implantitis
- Other Services
- Other Services
- Soft Tissue Grafting
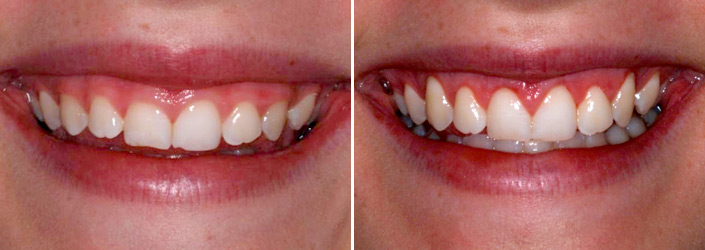
- Crown Lengthening
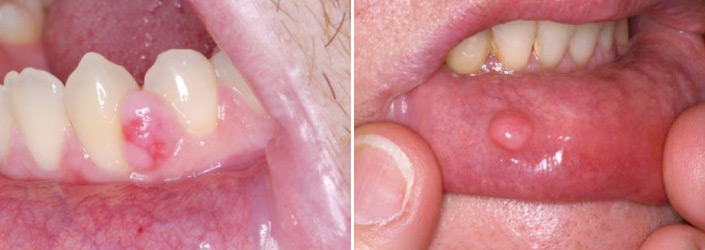
- Biopsies
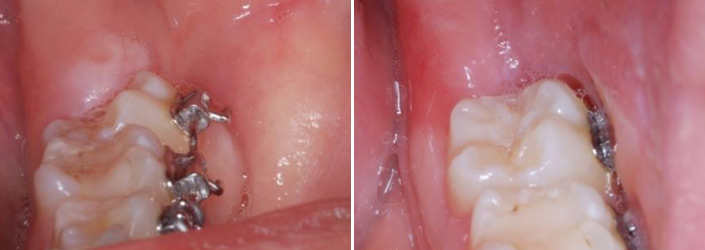
- Bone Grafting/Regeneration
- Procedures to Help with Ortho
- Procedures to Help with Ortho
- Frenectomies
- Canine Exposure
- Gingivectomies
- Patient Info
- Patient Info
- FAQ
- Postoperative Instructions
- Resources
- Medical History Form
- Policies
- Referring Dentists
- Contact